Blocked Milk Ducts: What They Are, and How to Manage Them While Breastfeeding & Pumping
Author: Breast Physio Agnes Canadell
What is a blocked duct?
“It’s important to understand that this isn’t like a literal clog in a pipe, it’s more like a traffic jam of milk flow due to either swelling or insufficient drainage.”
Image: Little Bodhi Photography
Blocked milk ducts are one of the most common discomforts that breastfeeding parents encounter. Many describe them as painful lumps in the breast that make feeding uncomfortable but with the right care, most blocked ducts can be treated at home quickly and safely.
What Is a Blocked Milk Duct?
A blocked milk duct happens when milk is not draining effectively from part of the breast, which can create a small, tender lump. If untreated, this area of blocked milk can cause local inflammation and may progress along a spectrum toward more widespread breast inflammation (mastitis). (Mitchell et al, 2022)
It’s important to understand that this isn’t like a literal clog in a pipe, it’s more like a traffic jam of milk flow due to either swelling or insufficient drainage.
Signs and Symptoms
Blocked ducts often present with:
A tender, localised lump or area of firmness
Pain or discomfort in that area
Reduced milk flow on the affected side
Sometimes a milk bleb (white spot) on the nipple opening
Feeling generally uncomfortable without high fever
Blocked ducts usually do not cause fever. If you experience a high temperature or flu-like symptoms, this could be mastitis and should be assessed by a healthcare professional.
Old techniques just don’t work!
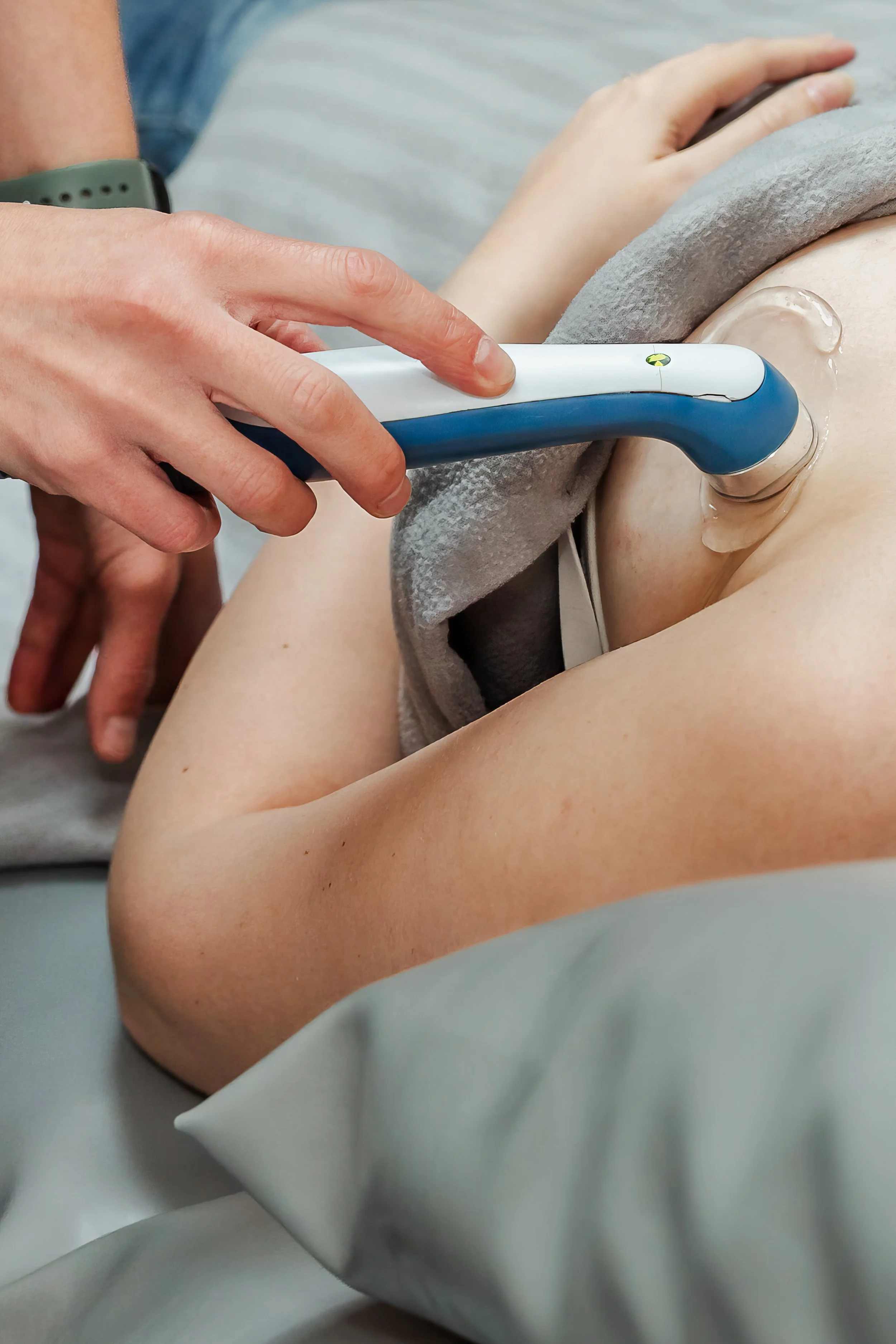
Therapeutic ultrasound (TUS), where clinically appropriate, to help soften and move the blockage within the duct to be fed or pumped out and progress the inflammatory response into the proliferation and remodeling phases quicker in the case of mastitis.
Image: Little Bodhi Photography
Evidence-Based Treatment & Management
Recent clinical guidance has shifted away from older recommendations like heat, vigorous massage or over-pumping, for most cases. Here’s the current expert-aligned approach:
1. Frequent Comfortable Feeding
Keep breastfeeding or expressing gently and regularly but don’t over-pump. The goal is comfort and regular milk removal, not exhaustion or overstimulation of the breast. (Mitchell et al, 2022)
2. Target Inflammation, Not Just Milk Removal
The ABM mastitis protocol emphasises reducing inflammation as the first step:
Ice packs on the sore area can reduce swelling and relieve pain.
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can help (discuss with your clinician).
Paracetamol may also provide pain relief. (ABM 2022 Protocol)
Heat is often still comfortable but can increase blood flow and swelling, so it’s usually not recommended as a primary treatment. (ABM 2022 Protocol)
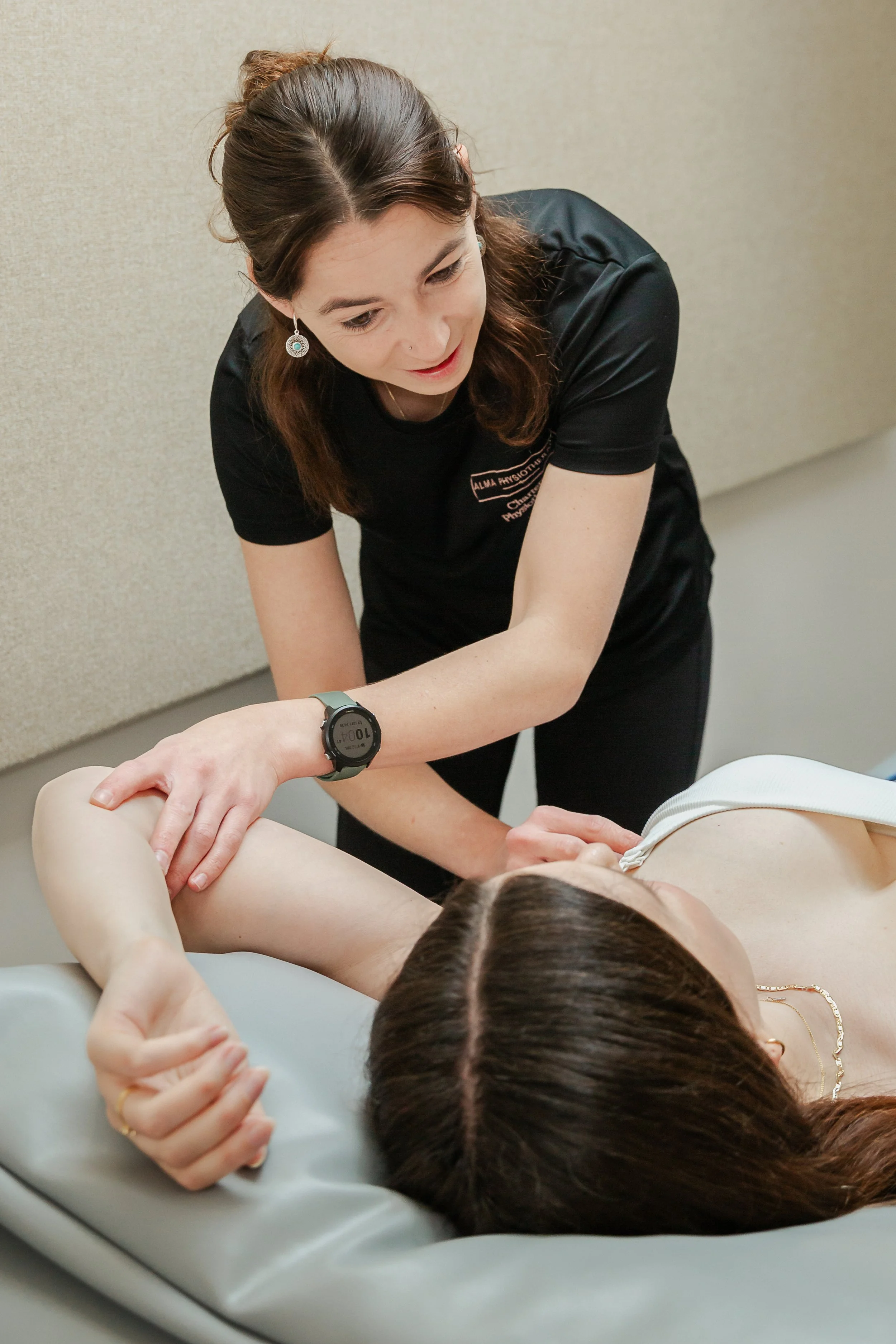
3. Gentle Approaches to Massage
If you choose to use massage, it should be light and gentle, working from the lump toward the lymphatic nodules to support lymphatic flow, not deep or forceful pressure.
4. Physiotherapy Supports
Seeking assessment from a physiotherapist trained in breastfeeding care early (ideally within the first 24 hours of symptoms) can help prevent progression along the mastitis spectrum.
Early support may include:
Therapeutic ultrasound (TUS), where clinically appropriate, to help soften and move the blockage within the duct to be fed or pumped out and progress the inflammatory response into the proliferation and remodeling phases quicker in the case of mastitis.
Lymphatic drainage approaches or taping to assist swelling reduction
Education on breast handling, positioning, bra fit, posture, and feeding mechanics
The goal is to calm inflammation, support comfortable milk flow, and reduce the likelihood of symptoms worsening, not to aggressively “clear a blockage.”
5. Use Warmth Before Feeding
Applying a warm compress or having a warm shower for a few minutes before feeding can help relax tissues and improve milk flow toward the nipple.
6. Check Clothing and Pump Fit
Ensure your bra or nursing wear isn’t compressing your breast. If you pump, make sure the flange size is correct as poor fit can hinder drainage.
7. Rest and Comfort
Give yourself permission to rest when you can; stress, fatigue and missing feeds can all contribute to milk flow issues.
What should you do?
Prompt assessment helps distinguish purely inflammatory mastitis from bacterial infection, which may require antibiotics. (NHS Guidelines)
Image: Little Bodhi Photography
What Not to Do
Avoid:
Vigorous massage or squeezing that increases inflammation
Excessive pumping beyond what is comfortable or needed
Using heat as the main treatment (because it may worsen swelling)
Initiating antibiotics without clear signs of infection
The emphasis now is on evidence-based inflammation management, not aggressive milk drainage.
What has changed?
The emphasis now is on evidence-based inflammation management, not aggressive milk drainage.
Image: Little Bodhi Photography
When to Seek Medical Help
You should contact a healthcare professional if:
Symptoms don’t start improving after 24–48 hours
You develop fever or significant systemic symptoms
There’s a rapidly expanding painful red area
You suspect a breast abscess or harder lump
Pain is severe or worsening despite self-care
Prompt assessment helps distinguish purely inflammatory mastitis from bacterial infection, which may require antibiotics. (NHS Guidelines)
Blocked ducts and early inflammatory mastitis are not just “a clog”, they’re part of a broader process involving tissue inflammation. The latest clinical guidance highlights that reducing inflammation safely and supporting regular comfortable feeding is now the cornerstone of care. (ABM Protocol, 2022)
If you’re frequently dealing with painful lumps, pain, or inflammation while breastfeeding, a tailored physiotherapy assessment can help you manage symptoms and continue comfortable feeding.
Agnes is a sports, pelvic and breast health physiotherapist based at Alma Physiotherapy.
HCPC, POGP & CSP Registered
Click the button below to book an appointment or FREE 10 minute discovery call.
Email pa@almaphysiotherapy.co.uk or Whatsapp Kirsty to help you book in +447942 494506
(Image: Little Bodhi Photography)
References
ABM 2022 Protocol - The Mastitis Spectrum, MASTITIS SPECTRUM RECOMENDATIONS: “ANTICIPATORY GUIDANCE AND BEHAVIOURAL INTERVENTIONS” (ABM)
Lin KY et al (2023). Physical therapy intervention for breast symptoms in lactating women: a randomized controlled trial. BMC Pregnancy Childbirth. 14;23(1):792. doi: 10.1186/s12884-023-06114-2.
Mitchell KB, Johnson HM, et al. (2022). Academy of Breastfeeding Medicine Clinical Protocol #36: The Mastitis Spectrum, Revised 2022. Breastfeeding Medicine. Academy of Breastfeeding Medicine.
NHS (UK). Mastitis – Symptoms and Treatment Guidance.